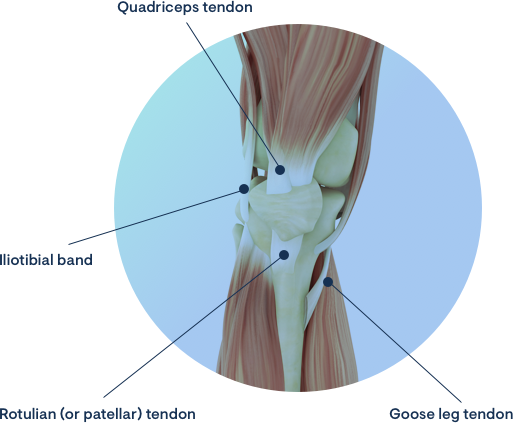
Knee Tendonitis
Tendonitis of the knee is the inflammation of the tendons that exist around the knee joint, often leading patients to seek out their knee specialist doctor. They are a frequent cause of knee pain and generally result from situations of overstraining, namely those that occur during sports practice, whether in high competition athletes or weekend sportspeople.
The diagnosis is made, primarily, by discriminating the characteristics of the pain, specifying: the location; the inflammatory nature; the triggering factor (usually high intensity exercise) and the response of this condition to anti-inflammatory medication, rest and ice.
Oedema and tumefaction may sometimes be visible in the area affected by tendonitis and palpation of the pain site can help identify the knee structure affected by tendonitis.
Usually, as auxiliary diagnostic tests, ultrasound and MRI of the knee are used, due to their high sensitivity and specificity to identify soft tissue pathology. Radiological examinations may reveal axial deviations of the lower limbs which are also an etiological factor, as well as small calcifications in the tendon insertions (the so-called enthesopathies).
The treatment for knee tendonitis, in general, involves reducing physical activity (or even resting), anti-inflammatory drugs and ice packs.
A rehabilitation programme (physiotherapy) adapted and prepared by your specialist in physical medicine and rehabilitation is important to speed up the process of recovery and eventual return to sport.
Surgery is rarely indicated for the treatment of tendonitis, which is why it should be carefully considered by your orthopaedic surgeon. It is reserved for chronic tendinopathies that are resistant to conservative treatment and have associated partial or complete ruptures.
See below specifically which are the most frequent tendonitis/bursitis of the knee and how to treat them individually:
The diagnosis is made, primarily, by discriminating the characteristics of the pain, specifying: the location; the inflammatory nature; the triggering factor (usually high intensity exercise) and the response of this condition to anti-inflammatory medication, rest and ice.
Oedema and tumefaction may sometimes be visible in the area affected by tendonitis and palpation of the pain site can help identify the knee structure affected by tendonitis.
Usually, as auxiliary diagnostic tests, ultrasound and MRI of the knee are used, due to their high sensitivity and specificity to identify soft tissue pathology. Radiological examinations may reveal axial deviations of the lower limbs which are also an etiological factor, as well as small calcifications in the tendon insertions (the so-called enthesopathies).
The treatment for knee tendonitis, in general, involves reducing physical activity (or even resting), anti-inflammatory drugs and ice packs.
A rehabilitation programme (physiotherapy) adapted and prepared by your specialist in physical medicine and rehabilitation is important to speed up the process of recovery and eventual return to sport.
Surgery is rarely indicated for the treatment of tendonitis, which is why it should be carefully considered by your orthopaedic surgeon. It is reserved for chronic tendinopathies that are resistant to conservative treatment and have associated partial or complete ruptures.
See below specifically which are the most frequent tendonitis/bursitis of the knee and how to treat them individually:
